Bilateral Total Knee Arthroplasty in Hemophilia Patients is Safe and Cost-Effective, Study Suggests
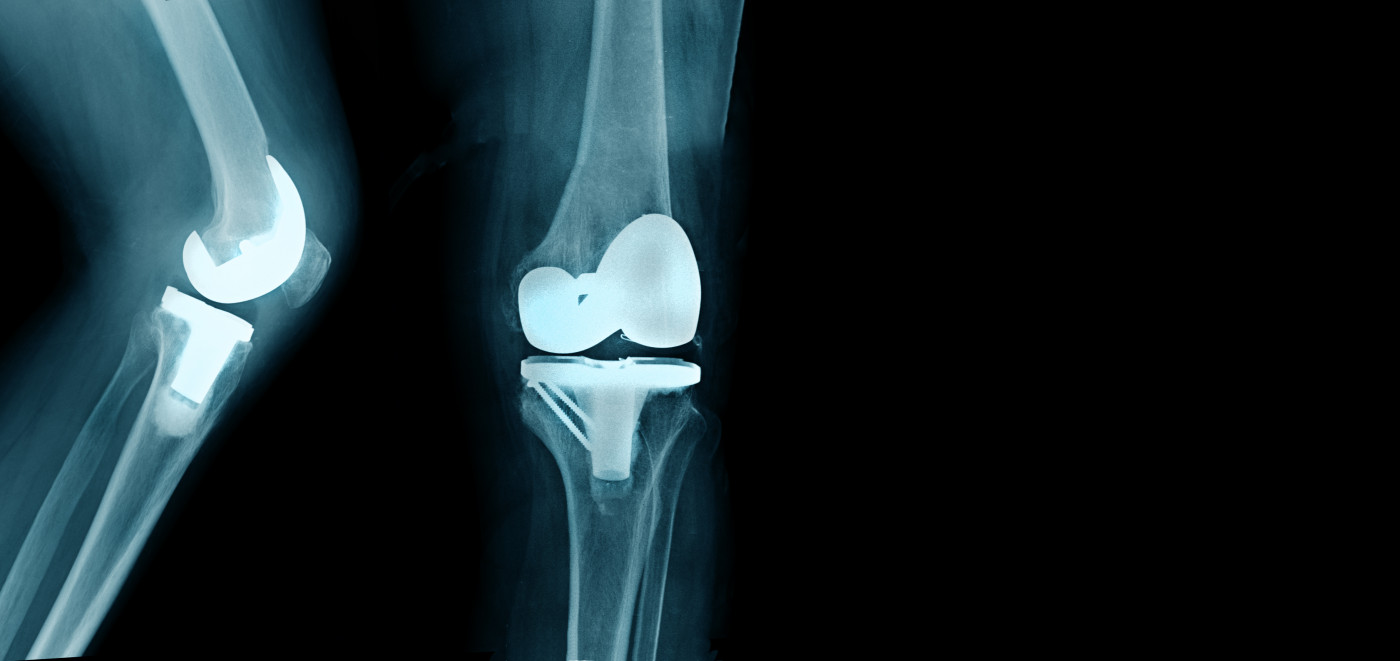
New research shows that bilateral total knee arthroplasty — or reconstruction of the joint — is a safe and cost-effective treatment for patients with hemophilic arthropathy (a hemophilia degenerative joint disease).
The study, titled “Simultaneous bilateral total knee arthroplasty in patients with end-stage hemophilic arthropathy: a mean follow-up of 6 years,” was published in Nature Scientific Reports.
Hemophilic arthropathy is a common complication that affects more than 90 percent of patients with hemophilia. It results from repeated hemarthrosis, which refers to bleeding into joint spaces. Often, multiple joints, such as the knee and hip, become affected, leading to loss of function and permanent disabilities.
The best approach to prevent hemophilic arthropathy is to administer regular factor replacement therapy. Unfortunately, 70–80 percent of patients with hemophilia cannot receive appropriate treatment and are at increased risk of developing hemophilic arthropathy. The knee joint, in particular, is vulnerable to this condition.
In order to treat hemophilic arthropathy of the knee, total knee arthroplasty (TKA) is considered a good option. Factor replacement therapy is important during surgery to maintain an adequate level of clotting factors in the body to minimize blood loss.
Often, both knees are involved, and therefore bilateral TKA has to be conducted. However, staged bilateral TKA— performing surgery on each knee separately over a specific time interval — requires repeated clotting factor infusions. That could lead to the development of inhibitors against coagulation factors, as well as higher hospitalization costs. Researchers postulated that simultaneous bilateral TKA may be considered a better treatment option.
They conducted a retrospective study of 36 patients with a mean follow-up of 6 years to investigate the safety, cost-effectiveness, and medium- and long-term clinical outcomes of patients who received simultaneous bilateral TKA compared to unilateral TKA.
The scientists assessed parameters such as requirements for transfusions, complications, costs, hospital stays, Hospital for Special Surgery (HSS) knee scores, knee range of motion (ROM) and revision rates.
Results showed that patients who underwent bilateral TKA did not require more transfusions or consumption of coagulation factors compared to patients who had unilateral TKA. Furthermore, complications were observed in 13 of 36 patients who underwent bilateral TKA, compared to six of 18 patients in the unilateral TKA group, which was not statistically different.
The hospital stay for patients who underwent unilateral TKA was an average of 29.11 days compared to 32.39 days for patients who had bilateral TKA — again, not a significant difference.
The cost of hospitalization (excluding the prosthesis) was an average of $14,945.41 for the bilateral TKA group compared to $14,742.12 for the unilateral TKA group, which also was not significantly different.
Finally, the two groups exhibited similar medium-term knee HSS scores and ROM.
The authors wrote, “Our data indicate that bilateral TKA is a safe and cost-effective treatment for HA with similar medium-term results compared to unilateral TKA.” However, the authors add that further large-scale studies will have to be conducted to obtain a definite conclusion.





