Manual Therapy With Passive Stretching Helps Hemophilia Patients’ Joints, Study Finds
Written by |
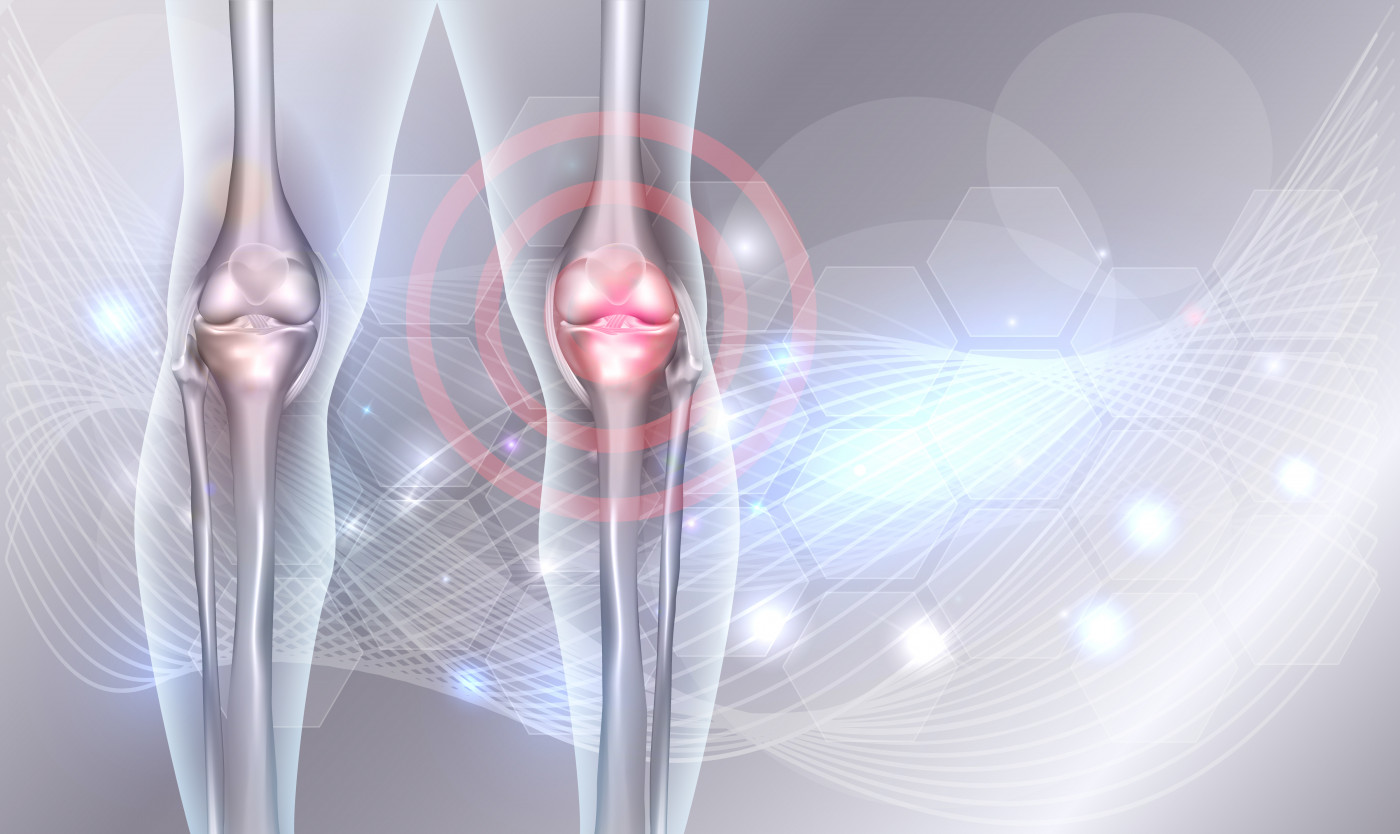
Manual therapy, in combination with passive stretching, can reduce the frequency of joint bleeds and improve joint health in people with hemophilia, a small study shows.
The study, “The effectiveness of manual therapy in addition to passive stretching exercises in the treatment of patients with haemophilic knee arthropathy: A randomized, single‐blind clinical trial,” was published in the journal Haemophilia.
Bleeding into a joint, termed hemarthrosis, can occur as a symptom of hemophilia. This can result in joint disease called hemophilic arthropathy, which can be painful and substantially impair movement.
Management of joints in people with hemophilia requires multidisciplinary care. In addition to pharmacological treatments, physiotherapy — stretches and other exercises to improve joint health — is an important part of hemophilia joint management. Manual therapy is a type of physiotherapy that involves having a therapist use their hands to manipulate parts of the body.
Because of its load-bearing position in the body, the knee is a common site of hemarthrosis in people with hemophilia. But, even though knee arthropathy is common in patients with hemophilia, few studies have assessed the effectiveness of manual therapy applied to this joint.
A team of researchers from Spain hypothesized that adding manual therapy to passive stretching (stretching by holding one position for a length of time) would improve joint health in people with hemophilia. Prior results of their clinical trial (NCT02198014), sponsored by Universidad Católica San Antonio de Murcia, showed that home-based physiotherapy eased pain perception in the ankle and improved quality of life in hemophilia patients.
The researchers now analyzed 28 participants (mean age 31 years, 24 with type A and four with type B) who had arthropathy of the knee. Participants experienced a mean of 1.61 knee hemarthroses in the three months before the start of the study.
Half of the participants, serving as controls, were asked to follow their normal routine over the course of the study. The other half received manual therapy in combination with passive stretching, for two hour-long sessions per week, for 12 weeks.
Participants were assessed before and after treatment, then again at a follow-up 12 weeks later (at nearly six months).
In the control group, the mean frequency of joint bleeding in the knee was 0.71 after treatment and 2.29 at follow-up. In the group that received therapy, these rates were markedly lower: 0 after treatment and 0.43 at follow-up. Relative to the start of the study, the frequency of knee hemarthrosis decreased significantly in the group that received therapy, both immediately after the study and at follow-up.
Participants’ joint pain, rated on a scale from 0 to 10, decreased significantly in the therapy group: from a mean of 5.21 before the study, to 2 after 12 weeks, to 1.71 at follow-up. In contrast, pain scores in the control group did not change significantly.
Likewise, the therapy group showed evidence of improved joint health and increased range of motion in the knee. No such benefits were seen in the control group.
“Manual therapy improves joint health, range of motion and perceived pain in patients with haemophilic knee arthropathy. Six months after treatment, improvements are maintained in these patients,” the researchers concluded.
Notably, concerns have been raised previously that physiotherapy could increase the risk of bleeding in people with hemophilia. However, the results of this study suggest that the opposite is true, since hemarthrosis frequency decreased in the group given manual therapy. According to the investigators, this could be due to the physical effects of therapy, such as reducing pressure within the joint.
This study’s main limitation is the small sample size, said the investigators. In addition, some factors that might be of relevance — for instance, strength and quality of life — were not assessed.
“Future randomized clinical trials, with a larger sample size, should confirm the results of this study,” the scientists wrote. “The inclusion of variables such as functionality, strength and quality of life would offer a more global view of the efficacy of interventions in patients with haemophilic knee arthropathy.”


Leave a comment
Fill in the required fields to post. Your email address will not be published.