Gene Therapy Seen to Produce FVIIa Levels Needed to Control Bleeding in Rat Study of Hemophilia A
Written by |
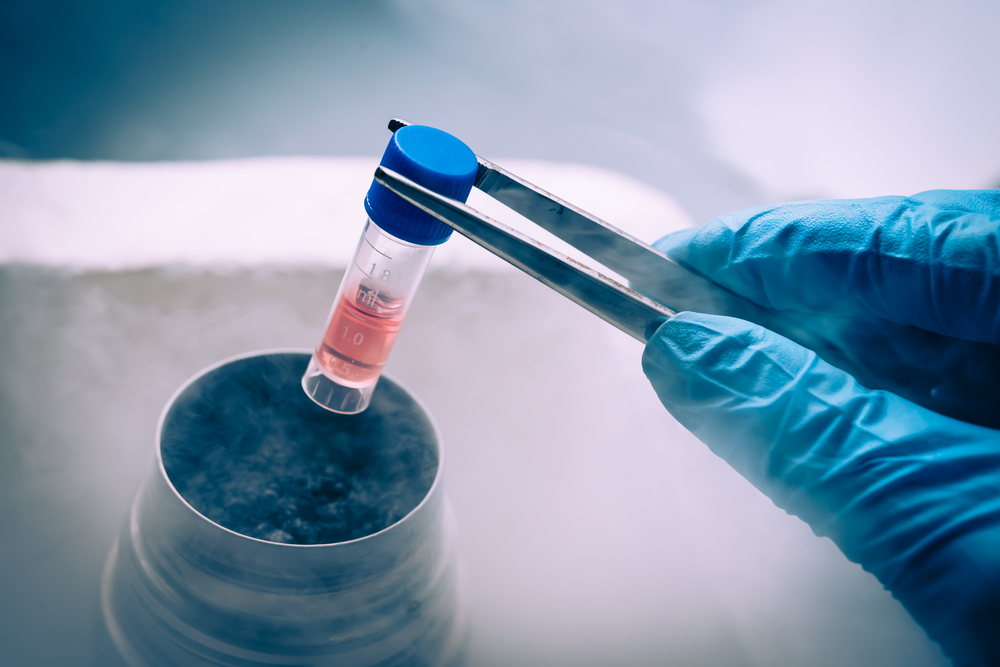
A gene therapy-based factor VIIa (FVIIa) given as prophylactic, or preventative, treatment was seen to produce specific factor levels needed to reduce the frequency of spontaneous bleeding episodes in a rat model of hemophilia A.
According to scientists, this work may be a first step in developing therapies that bypass a long-standing issue with prophylactics: the production of antibodies (inhibitors) that prevent clotting factors from working in given patients. This FVIIa treatment approach may also help those with hemophilia B, and work in both patient groups regardless of inhibitors.
The study, “Gene-based FVIIa prophylaxis modulates the spontaneous bleeding phenotype of hemophilia A rats,” was published in Blood Advances.
Hemophilia is a genetic disorder affecting blood clotting necessary to prevent excessive bleeding. In hemophilia A, this inability is caused by the lack of a specific clotting protein in blood, called factor VIII (FVIII), and it is treated with intravenous infusions of manufactured FVIII. But a third of hemophilia A patients will develop an immune response that renders the treatment useless.
“Patients who develop antibodies to the coagulation factors usually prescribed for hemophilia have a complicated treatment,” called a bypass approach using other compounds including factor VIIa, Paris Margaritis, PhD, a hematology researcher in the Raymond G. Perelman Center for Cellular and Molecular Therapeutics at Children’s Hospital of Philadelphia (CHOP) and study lead author, said in a news release.
“A different factor, called coagulation factor VIIa, restores blood clotting when given after a bleed occurs,” she added, “but we don’t know the target level of circulating factor VIIa that would prevent bleeds before they start. Our new preclinical results are the first to show target levels that could act prophylactically.”
Furthermore, while “current clinical data on the efficacy FVIII or FIX gene therapy for hemophilia are encouraging … no data exist on inhibitor patients,” the study said. But work in animal models show that an “VIIa-transgene approach may also be a suitable gene therapy alternative” in treating this patient group.
To determine a safe therapeutic threshold for FVIIa, Margaritis and his team used a rat model of hemophilia A provided by Novo Nordisk, the pharmaceutical company that is also the largest producer of artificial FVIIa used as a bypass strategy in patients with hemophilia A.
They used a harmless virus (called a viral vector) as a transport tool to deliver different amounts of a working FVIIa gene to groups of sick animals. All animals were then monitored for 17 weeks to assess the frequency of bleeding episodes and the corresponding levels of FVIIa in their blood, and outcomes compared with an untreated control animal group.
Results showed that while 91% of untreated rats had at least one spontaneous bleeding episode, similar episodes were seen 83% of treated animals producing up to 708 ng/ml of rat FVIIa, and 33% of those producing more than 708 ng/ml of FVIIa.
Treated rats producing more than 1250 ng/ml of the FVIIa transgene experienced no bleeds throughout the study.
On average, animals with at least 708 ng/ml of the FVIIa transgene also bled less after an injury (1.92 ml) compared to untreated animals (13.69 ml), with that loss “sufficient to normalize the blood loss after a tail vein injury,” the researcher reported, meaning a blood loss comparable to that seen in healthy rats with such an injury (1.11 ml).
No adverse events directly linked to this gene therapy were reported during the study.
“For the first time, we have threshold levels of factor VIIa for prophylactic use,” Margaritis said. “Because factor VIIa bypasses the need for factor VIII or IX, it should work in both hemophilia A and hemophilia B. Furthermore, it works whether or not inhibitors are present in the blood.”
“Clinical observations will need to validate our data” and test it in studies with patients, the scientists concluded, adding, “we believe that our approach combined with the animal model and obtained data will be useful in future studies toward that goal.”



Manpreet
Please work on it fast, people needed cure .
Moayad aziz
I hope to catching the new solution to end suffering of blood bleding
I have 3sons im from iraq
009647801212549